The effectivity of pharyngeal strengthening exercise, hyolaryngeal complex range of motion exercise, and swallowing practice in swallowing function of ischemic stroke patients with neurogenic dysphagia
Article information
Abstract
Dysphagia is associated with an increased risk of aspiration pneumonia which often results in death in stroke patients. Therefore, effective and efficient management is important. Behavioral therapy for swallowing rehabilitation based on the principles of neuroplasticity such as oropharyngeal strengthening and range of motion exercises are the alternative ones that often be used. This study aimed to assess the changes in swallowing function in ischemic stroke patients with neurogenic dysphagia after pharyngeal strengthening exercise, hyolaryngeal complex range of motion exercise and swallowing practice. Swallowing function was assessed using Penetration Aspiration Scale (PAS) and Functional Oral Intake Scale (FOIS) based on Flexible Endoscopic Evaluation of Swallowing before and after interventions. The interventions were given every day with a duration of 30–45 minutes for 4 weeks. There were six subjects who completed the study. The PAS before the interventions were 6.00±1.79 and after the interventions was 1.67±0.82 (P=0.003). Meanwhile, the FOIS score before the interventions was 3 (1–5) and after the interventions were 5.00±2.10 (P=0.041). There was an improvement of PAS and FOIS after the interventions. Therefore, the interventions can be suggested to be used as one of the treatments to improve swallowing function in ischemic stroke patients with neurogenic dysphagia.
INTRODUCTION
Dysphagia occurs in 50%–60% of patients who experience cerebrovascular lesions due to stroke. Half of patients who experience dysphagia are proven to have aspiration and 20%–30% of them develop aspiration pneumonia (Shaker and Geenen, 2011). Aspiration pneumonia is the most frequent respiratory complication which results in death in stroke and becomes the most frequent cause of repeated treatment in stroke patients for up to 5 years after stroke attack (Hegland et al., 2016). In 2018, at the Endoscopic Clinic of the Department of Ear Nose and Throat-Head and Neck Surgery RSUPN Ciptomangunkusumo, there were 346 patients with oral and pharyngeal neurogenic dysphagia who performed Flexible Endoscopic Evaluation of Swallowing (FEES), 82 of which were caused by stroke (Departemen Telinga Hidung Tenggorok Kepala Leher Rumah Sakit Ciptomanunkusumo, 2018).
Therefore, effective and efficient management becomes important. Conventional dysphagia rehabilitation includes the administration of several maneuvers and strategies to improve the safety of swallowing and protect the airway. This therapy is often given in conjunction with modified food and drinks consumed so that an effective and efficient process of eating and swallowing is achieved (Carnaby and Harenberg, 2013; Malandraki et al., 2016). The therapeutic effect is temporal and adherence to therapy is very low. Conversely, swallowing rehabilitation behavioral therapy such as strengthening exercises and movement exercises are alternatives that are often used. This therapy is more directed at the underlying physiological deficits so that therapeutic effect can last longer (Malandraki et al., 2016).
After a stroke, rehabilitation of sensorimotor functions such as swallowing gets good result through a variety of exercises based on learning experiences which, if repeated, can modify the structure and function of neurons and synapses in the brain (Kleim and Jones, 2008; Robbins et al., 2008). Therapies which include training on these swallowing organs are based on the principle of neuroplasticity which depends on experience and/or physiological guidelines for exercise (Carnaby-Mann and Crary, 2010; Crary et al., 2012). Some of these therapies, such as those developed by Malandraki et al through Intensive Dysphagia Rehabilitation, have shown positive outcomes. This therapy includes three components: oropharyngeal training, practice of swallowing, and things that increase compliance. Oropharyngeal exercises include tongue strengthening exercises, pharyngeal strengthening exercises through effortful swallow, basic tongue movement exercises through tongue-hold maneuvers and hyolaryngeal complex range of motion exercises through Mendelsohn maneuver. This approach is able to improve physiological swallowing and increase functional output in patients with neurogenic dysphagia (Malandraki et al., 2016).
Previously, preliminary research had been conducted to determine the type of exercise and the outputs that were able to carry out in this study. In June 2018, a cross-sectional study was done by looking at medical records and FEES results in 11 stroke patients with neurogenic dysphagia. The majority of features of FEES abnormalities found were standing secretion, penetration and aspiration, residue and reduced hypopharyngeal sensitivity. Based on these results, pharyngeal strengthening exercise through effortful swallow and hyolaryngeal complex range of motion exercise through Mendelsohn maneuver and repeated swallowing practices were chosen as interventions to be conducted in this study.
At present, in Indonesia, there are no studies that have applied Intensive Dysphagia Rehabilitation in stroke patients with neurogenic dysphagia, so it is not yet known whether this rehabilitation program can improve swallowing function in ischemic stroke patients with neurogenic dysphagia. This research will be carried out by applying some parts of Intensive Dysphagia Rehabilitation to determine changes in swallowing functions as assessed by Penetration Aspiration Scale (PAS) and Functional Oral Intake Scale (FOIS) based on FEES examination in patients with ischemic stroke with neurogenic dysphagia after doing pharyngeal strengthening exercise, hyolaryngeal complex range of motion exercise and swallowing practices.
MATERIALS AND METHODS
This research is an intervention study using pre and post design methods, comparing subjects with ischemic stroke with neurogenic dysphagia before and after the intervention of pharyngeal strengthening exercise, hyolaryngeal complex range of motion exercise and swallowing practices for 4 weeks. The study was conducted at the Medical Rehabilitation Clinic RSUPN Ciptomangunkusumo, Jakarta in July 2018 to February 2019. The sample size was six people. Criteria for acceptance of subjects are: (a) male or female aged 40–70 years; (b) diagnosed with ischemic stroke and in a subacute phase, conscious, and hemodynamically and neurologically stable; (c) able to sit upright for 30–40 min; (d) diagnosed with oropharyngeal neurogenic dysphagia established from a FEES examination at the last 3 months accompanied by one of the following criteria: a score ≥3 on the PAS or a score ≤5 on FOIS; (e) good cognition with Mini-Mental State Examination (MMSE) that has been adjusted for age and education; (f) cooperative and willing to participate in this study by signing an informed consent sheet after getting explanation; (g) have caregiver who have good cognition (MMSE ≥27), willing to participate and cooperative to ensure the patients do the swallowing rehabilitation according to the research protocol. Criteria for rejection of the subject are: (a) have neurological disorders or other conditions that may cause dysphagia, (b) there are language disorders, hemineglected, hemiinattention. Subjects were declared dropped from the study if: (a) do not do the exercise for more than 3 consecutive days in 1 week, (b) do not do the exercise 6 times or more, (c) withdraw from the study.
This research protocol was declared to have passed an ethical review by Research Ethics Commission of the Faculty of Medicine, University of Indonesia (0260/UN2.F1/ETIK/2018). This research was conducted by following ethical norms, those are all subjects were given explanation of the objectives, benefits and procedures of the study.
The outcomes assessed in this study are PAS and FOIS. PAS is a scale of 8 points, aimed to determine the severity of penetration and aspiration during a video fluoroscopic examination of swallowing. This scale is based on the distance of food material enter the airway or the level of cleanliness of the airway from food material (Butler et al., 2015). FOIS is a scale that reflects the functional level of oral intake of patients with dysphagia. This scale consists of seven levels and is very useful in documenting clinical changes and can be used independently in assessing the functional oral intake of dysphagia patients (Crary et al., 2005).
Numerical data normality test in this study was carried out using Saphiro–Wilk test. Data were then analyzed based on paired numerical comparative analyzes (repeated measurements). Analysis of normally distributed data uses the paired t-test, whereas the data that not normally distributed are analyzed using the Wilcoxon test.
The total sample in this study that met the acceptance criteria and did not meet the rejection criteria and followed the study to completion was six people. This amount was sufficient for the minimum number of sample calculations previously determined.
RESULTS
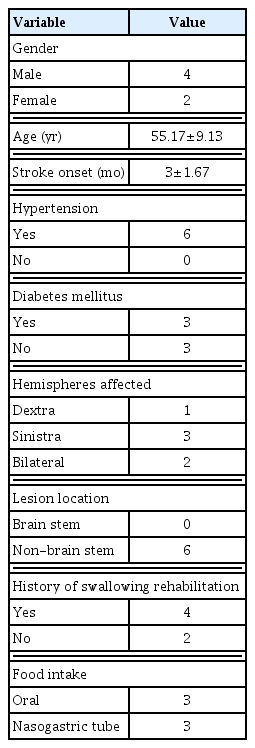
The characteristics of subjects in this study have been described in Table 1. Of the six subjects of this study, four were male, with a mean age of subjects was 55.17±9.13 years. The mean onset of stroke was 3.0±1.67 months. All subjects experienced dysphagia since the onset of stroke occurred. Two of six subjects had lesion in both hemispheres. Only one subject had lesions in the right hemisphere and the rest had lesions only in the left hemisphere. The location of the lesion of all subjects was not in the brain stem, with predominant subcortex involvement. Three of the six subjects could still get food and drink intake orally, while the other three subjects had to use nasogastric tube (NGT).
When evaluating FEES before intervention, in the preswallowing assessment, there were standing secretions in the vallecula, pyriformis sinus and post cricoid in all subjects. As described in Table 2, Two of six subjects had penetration and there were no aspirations in all subjects. In swallowing assessment using five types of food consistency, two of six subjects had only penetration and residue that could be overcome by repeated swallowing movements and adequate cough reflex. Conversely, the four subjects had aspirations and they had to use NGT. However, one of these four subjects, the aspirations occurred could be overcome by certain position of swallowing and had sufficient cough reflexes so that it was still possible to obtain food and drink intake orally.
From the results of the FEES evaluation before the intervention in Table 3, the mean PAS was 6.00±1.79. Meanwhile, the median of functional level of oral intake as assessed by FOIS was three, minimum value was one and maximum value was five. Quantitatively, there was an improvement in PAS with the mean PAS after intervention was 1.67±0.82. This change was statistically significant with P=0.003. The mean PAS change in this study was 4.33±1.97. This was in line with FOIS improvement which the mean after intervention was 5.00±2.10. The change in FOIS before and after intervention was also statistically significant with P=0.041 and mean change of FOIS was 2.00±1.67.
DISCUSSION
The mean improvement of PAS in this study was 4.33±1.97. Kim et al. (2017) conducted a study combining effortful swallow with Mendelsohn maneuver as an exercise in poststroke dysphagia patients. From the results of this study, the combination of these programs was able to improve PAS±2 points (Kim et al., 2017). Malandraki et al. (2016) also applied a combination of effortful swallow and Mendelsohn maneuver in dysphagia patients for 4 weeks and obtained an improvement of PAS 2.36 points (Malandraki et al., 2016).
Some researchers claimed that delayed initiation of pharyngeal swallowing is an important indicator of aspiration in stroke survivors (Mann et al., 1999; Power et al., 2007). Aspiration is also related to incomplete laryngeal closure due to reduced hyoid and laryngeal elevation. Laryngeal closure is largely determined by arytenoid and epiglottic cartilages to protect the airway. Reduced elevation of the hyoid and larynx is an independent indicator of aspiration. It is known that elevation of the hyoid and larynx will result in a shift of the hyoid bone anteriorly and superiorly during the swallowing phase. When the bolus passes through the pharynx, the base of the tongue which is the attachment of the hyoid bone will pull the hyoid bone and larynx anteriorly and superiorly so that an epiglottal retroflection movement will protect the airway. In addition, this epiglottic movement will also open the upper esophageal sphincter so that the bolus can enter the esophagus (Han et al., 2016; Matsuo and Palmer, 2008; Pearson et al., 2013). A decrease in hyoid elevation was very closely related to epiglottic immobility and subsequently results in penetration and aspiration (Carnaby-Mann and Crary, 2010).
From the results of the FEES examination prior to the intervention, all subjects had standing secretion during preswallowing assessment and residue during swallowing. Pharyngeal constriction is one of the parameters used to differentiate normal swallowing functions from impaired swallowing functions. Dejaeger et al. (1997) concluded that posterior tongue thrust, pharyngeal shortening, and pharyngeal constriction play a role in determining the presence or absence of residues after swallowing. The posterior thrust of the tongue was said to be strongly related to residues in the vallecula, whereas shortening and constriction of the pharynx are related to residues in pyriformis sinus (Stokely et al., 2015). Pharyngeal strengthening exercise through effortful swallow is designed to increase the basic motion of the tongue to the posterior and also the pharyngeal wall movement to anterior so that, there will increase the pressure for pushing the bolus and then reduce pharynx residual (Fukuoka et al., 2013; Palmer et al., 2000). Movement of the bolus during swallowing depends on the synergistic action of the oropharyngeal propulsion and hypopharyngeal suction. The greatest oropharyngeal propulsion force is caused by contact pressure between the tongue and the hard palate during ingestion of the oral phase. Contact that occurs between the anterior part of the tongue and the palate becomes an important part of tongue movement which will keep the bolus in the oral cavity and ensure proper transport of the bolus. Fukuoka et al. (2013) evaluated the tongue pressure against the hard palate during swallowing with effortful swallow and obtained increased results when compared to normal swallowing without effortful swallow. Huckabee et al. (2008) said that tongue pressure to the palate during effortful swallow will increase submental activation, orolingual pressure, and upper pharyngeal pressure. Increased oral pressure will also increase pharyngeal pressure and movement so it will capable of pushing the bolus from the oral cavity to the pharynx (Fukuoka et al., 2013).
Not only effortful swallow, Mendelsohn maneuver is also related to standing secretions and residues during the swallowing phase. Slightly different, this maneuver is able to extend and strengthen tongue-palate contact pressure especially in the posterior part, even the pressure caused by effortful swallow remains better. This is important in elevation of hyoid and larynx during swallowing, so that the duration of movement of the larynx to the anterior and superior will increase and prolong the opening of the upper esophageal sphincter (Fukuoka et al., 2013).
Mendelsohn’s maneuver is one of the therapies that use the principle of voluntary prolongation of laryngeal elevation at peak of swallowing. Some studies said that Mendelsohn maneuver as a compensation strategy was able to increase laryngeal elevation and hyoid movement to the anterior and superior so that the cricoid cartilage will be pulled. McCullough and Kim (2013) stated that this maneuver not only improves the bolus transit time quickly, but also able to improve swallowing coordination.
Disability caused by penetration and aspiration was assessed through FOIS which showed the functional level of the subject’s oral intake. The mean improvement in FOIS in this study was 2.00±1.67 points. The improvement of FOIS was in line with the improvement of PAS. The functional level of oral intake was surely related to PAS. The reduced amount of penetration and/or aspiration in the subjects after the intervention clearly had a positive impact on the functional level of oral intake. The absence of aspiration in the FEES examination after the intervention was a contributing factor in FOIS improvement. Crary et al. (2016) stated that there was an improvement in FOIS as expected in stroke patients for up to 6 months in the recovery period.
After the intervention, one in six subjects still used NGT and there were no FOIS changes before and after intervention. This is due to an inadequate cough reflex and the risk of postswallowing aspiration. This made no improvement of FOIS even there was improvement of PAS.
An inadequate cough reflex is a risk for silent aspiration. As known, coughing is a very important body defense mechanism to increase the excretion of particles and to protect the airway from aspiration and foreign materials. Coughing occurs through complex reflex arch stimulation. Starting from the irritation of cough receptors in the trachea, carina, large airway branches, distal airway and also in the pharynx. The cough reflex consists of: (a) the afferent pathway, contains sensory nerve fibers that carry impulse to the medulla, (b) the central pathway, located in the upper brain stem and pons, and (c) the efferent pathway, continue impulse from the cough center to the diaphragm, abdominal wall and muscles. In stroke patients, one of these cough reflex pathways can be disrupted, resulting in an inadequate cough reflex and leading to aspiration (Polverino et al., 2012). Effortful swallow and Mendelsohn maneuver in this study did not aim to improve the cough reflex, but they were proven improved PAS and reduced the risk of penetration and/or aspiration. This improvement was also seen in the functional level of oral intake assesses by FOIS.
Oropharyngeal exercises and repeated swallowing practices performed in this study are based on the principle of neuroplasticity. Sessle et al. (2005) reported that during the 1–2 months period of tongue protrusion exercise, the sensorimotor cortex region which is given intracranial stimulation became widespread. The study also showed that the proportion of primary motor cortex neurons and primary somatosensory cortex increased significantly after tongue protrusion exercises (Martin, 2009; Robbins et al., 2008). The expansion of the cortex region due to protrusion of the tongue was in accordance with the concept of neuroplasticity “use it” and “improve it.” This was also consistent with the concept of specificity which stated that the region of the body competes for its representation in the cortex and the use of the body part could increase its representation (Robbins et al., 2008). This frequent and repetitive stimulation was one of the bases for intervention in this study, according to the principle of neuroplasticity.
From the results of this study, there was improvement in PAS and FOIS which was statistically significant in ischemic stroke patients with neurogenic dysphagia after pharyngeal strengthening exercise, hyolaryngeal complex range of motion exercise and swallowing practices for 4 weeks. Therefore, this intervention can be used as a treatment to improve swallowing function of stroke patients with neurogenic dysphagia.
Notes
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.