AbstractThere are many proposed core stability exercises in a variety of positions; however, it is not clear that in which position, activation of transverse abdominis muscle is utmost. We aimed to compare the activation of transverse abdominis muscle in different core stability exercise positions through ultrasound imaging. in a 20 subjects’ study we compared the effectiveness of drawing-in and bracing maneuvers on transverse abdominis in different core stability exercise positions (supine, hook lying, supine with 90° flexed knee and hip, supine with stretched knees and 90° flexed hips, bridge, bridge with one stretched knee and Bird dog). We used activation ratio and preferential activation ratio as measurements of transverse abdominis activation. Abdominal Bracing in the bridge position showed the highest activation of transverse abdominis (P<0.05). The results showed significantly higher activation of transverse abdominis, measured by preferential activation ratio, in bridge position during abdominal bracing.
INTRODUCTIONLow back pain is the most prevalent musculoskeletal problem; its lifetime and point prevalence are 58% to 84% and 4% to 33% respectively (Woolf and Pfleger, 2003). The loss of lumbar spinal stability is considered as a risk factor of low back pain (Panjabi, 1992). Transversus abdominis (TrA), the deepest abdominal muscles, plays major role in stabilization of lumbopelvic region (Willson et al., 2005). Reduced activation of the TrA has been linked to the incidence and progression of low back pain (Ferreira et al., 2004). On the basis of this, activation and strengthening of TrA have been suggested as possible therapeutic interventions in patients with low back pain (Panjabi, 1992; Selkow et al., 2017). The efficacy of these treatments has been shown in previous studies (Noormohammadpour et al., 2012; Noormohammadpour et al., 2018).
The rehabilitation approach toward low back pain usually includes core stability exercises to enhance the spinal stabilization (Hwangbo et al., 2015; Noormohammadpour et al., 2018). There are many proposed core stability exercises in variety of positions (supine, quadruped, etc.) Drawing-in and bracing are two principle maneuvers that are routinely used by conservative therapists for specific activation of abdominal muscles including TrA (Maeo et al., 2013). However, it is not clear that in which position, activation of TrA muscle through drawing-in and bracing maneuvers, is utmost.
An ultrasound (US) imaging study has been used as a technique for assessing TrA activation by measuring muscle thickness in resting and contraction states (Djordjevic et al., 2014). The reliability and validity of US imaging studies have been reported previously (Ehsani et al., 2016; Rostami et al., 2015). The aim of this study is to investigate and compare the effectiveness of drawing-in and bracing maneuvers in different core stability exercise positions (including supine, hook lying, supine with 90° flexed knees and hips, supine with stretched knees and 90° flexed hips, bridge, bridge with one stretched knee and bird dog) through US imaging.
MATERIALS AND METHODSWe conducted a comparative cross-sectional study to examine the activation of TrA in different core exercise positions.
ParticipantsWe asked 20 healthy volunteers with the age of 18 to 50 years who were screened for medical and medication history that could adversely affect muscle health or contraindicate testing included in the study. Exclusion criteria included self-reported history of low back pain in past 6 months and any previous musculoskeletal disease. We also excluded subjects who had practiced core training within past 6 months. All subjects received written and oral information about the study procedures before participation. Also, the study protocol was approved by the Ethical Committee of university (IR.TUMS.VCR.REC.1397.698). With the purpose of preventing measurement bias, all the participants were instructed not to consume meals or liquids 3 hr prior to measurement (Kordi et al., 2011; Noormohammadpour et al., 2015).
InstrumentOne musculoskeletal ultrasonography practitioner performed the US measures. Our investigator used a portable M-Turbo US system (FUJIFILM SonoSite Inc., Bothell, WA, USA) with a 13-MHz linear transducer to visualize and obtain an US image of lateral abdominal wall muscles including TrA during different positions.
Measurement positionsWe measured changes in muscle thickness of lateral abdominal wall muscles in resting condition and during both drawing-in and bracing in the following seven positions: supine, hook lying, supine with 90° flexed knee and hip, supine with stretched knees and 90° flexed hips, bridge, bridge with one stretched knee, and Bird dog. Fig. 1 shows the positions in which measurements were done. The participants performed a drawing-in maneuver by drawing the navel up and in toward the spine and maintaining the lumbar spine in a neutral position (Monfort-Pañego et al., 2009). The investigator also instructed participants to perform the bracing in maneuver by contracting the entire abdominal wall without any change in the position of the muscles and maintaining the lumbar spine in a neutral position (Monfort-Pañego et al., 2009).
MeasurementsThe transducer was being placed along the midaxillary, at the midway from the iliac crest and lower border of last rib. The transducer was adjusted to portray the best image quality, perpendicular to the skin surface. Two series of US images were obtained for each maneuver in each training position. We measured muscle thickness as the distance from the superior facial border to the inferior facial border of the muscle in millimeters after acquiring still B mode images. The investigator acquired images on the dominant side of each subject. In case of bird dog training position, the participants were instructed to use their nondominant side arm and dominant side leg. For US measurement at bridge position with the stretched knee, subjects were asked to stretch their nondominant side knee.
Outcome measurementsWe used activation ratio (AR) and preferential activation ratio (PAR) of TrA as final measurements of TrA activation in drawing-in and bracing maneuvers during different training positions. In this regard, AR was defined as maneuvered TrA thickness divided by rest TrA thickness and PAR was defined as a preferential increase in TrA thickness by doing the maneuver in compare to total lateral abdominal wall change.
The reliability of AR and PAR in the estimation of TrA thickness and their relevance with clinical outcomes have been shown in the previous study (McPherson and Watson, 2012; Mangum et al., 2016).
Statistical analysisThe normality of measured variables was assessed with Shapiro–Wilk test (Mishra et al., 2019). We have used paired sample t-test to compare the difference between activation measurements of drawing-in and bracing maneuvers in each core training position. To compare the results between different positions, analysis of variance (ANOVA) with repeated measures was used. All statistical analyses were conducted using IBM SPSS Statistics ver. 22.0 (IBM Co., Armonk, NY, USA).
RESULTSIn total, 25 subjects were invited but five participants were excluded before ultrasonography due to low back pain in last month (n=2), kyphosis (n=1) and practice of core training in the past 6 months (n=2). Finally, 20 participants completed the ultrasonography in all positions. Table 1 shows the demographic findings of subjects including age, gender, height, weight, and body mass index.
Table 2 presents measurements of TrA thickness during rest, abdominal drawing-in (AD) and abdominal bracing (AB) in different training positions. Table 3 reports the results of repeated measure ANOVA tests to compare the activation of TrA in different positions with AD and AB. AB in the bridge position showed the highest activation of TrA. Fig. 2 also can be used to compare AR and PAR of TrA in different positions.
DISCUSSIONOne of the most important functions of abdominal muscles is to increase trunk stability (Heidari et al., 2015; Norris, 1993). Therefore, designing any abdominal muscle exercises, one should consider the stabilizing roles of these muscles. The present study investigated TrA activation differences in drawing-in and bracing maneuvers in various core stability exercise positions through US imaging. The results show significantly higher activation of TrA, measured by PAR, in bridge position during AB. There has been substantial attention in the previous studies regarding the role of TrA as the deepest abdominal muscles (Ehsani et al., 2016), and the approach to train this muscle (Hodges, 1999; Noormohammadpour et al., 2012).
Patients with low back pain usually show a smaller increase in transverse abdominis thickness during their tasks. Similar results in EMG suggests impaired motor control of transverse abdominis among low back pain patients (Ekstrom et al., 2007). It has been indicated that the thickness of transverse abdominis muscle has correlation with its activity (Hodges and Moseley, 2003; McMeeken et al., 2004). That’s why TrA is one of the main targets of exercises aimed to prevent and rehabilitate low back pain. Drawing-in maneuver or AD aims to activate TrA while minimizing the contraction of other abdominal wall muscles such as the oblique muscles (Hodges, 1999). AB, on the other hand, has been suggested to activate the entire abdominal wall (Grenier and McGill, 2007). In this study, AB produced more TrA activity comparing to AD maneuver. Both AR and PAR of TrA were significantly higher during the AB maneuver. There is limited evidence comparing AB and drawing-in maneuvers in terms of TrA activation. In a recent study, these two techniques were compared in 20 young healthy male subjects while they were lying supine with their knee flexed (Kim and Lee, 2017) and EMG showed significantly more TrA activity during AD comparing to AB. One possible explanation for the different results could be the way subjects were instructed to perform AD in which in contrast to our study they were not asked to maintain their neutral spine position while performing the maneuver (Kim and Lee, 2017). In another study conducted by Kim et al. (2016), US was employed to measure muscle activation and thickness. In their study, TrA change ratio (TrA contract – TrA rest)/(TrA rest × 100) was calculated and compared between drawing-in and bracing. In terms of change ratio, drawing-in was greater than bracing. Additionally, all measures in Kim’s study were taken in the standing position, a position that was not assessed in our study. Computed tomography findings also show AD to be more effective in producing TrA contractions (Koh et al., 2014). Although some studies show better TrA activity during AD, our finding suggests otherwise. Measuring TrA elasticity using US it has also been documented that AB produces higher TrA elasticity comparing to six other training strategies including AD (Hirayama et al., 2017). The difference in the methods measuring TrA activity and subjects’ positions could be an explanation for these discrepancies.
The AR formula, calculated by dividing thickness in the contracted state by thickness at rest, is a measure of activation for TrA (Teyhen et al., 2005; Mangum et al., 2016). This measure helps clinicians determine the ability to activate the TrA. However, by taking into account only at rest and contracted states of TrA, this calculation cannot determine the ability to activate TrA alone without evoking a contraction of other abdominal wall muscles. Most rehabilitation programs focus on teaching the patients to contract TrA while keeping the external and internal abdominal oblique muscles, less contracted. The PAR formula, on the other hand, is calculated by measuring both thicknesses of TrA and the lateral abdominal wall muscles (Mangum et al., 2016; Mannion et al., 2008, Teyhen et al., 2005). This calculation helps to measure the patient’s ability to isolate spinal stabilizers such as TrA. Although PAR takes into account the entire lateral abdominal wall, AR seems to have higher reliability compared to PAR (Mangum et al., 2016). In this study, we found significant differences in AR and PAR of TrA during drawing-in maneuver between training positions, it was also the case for PAR of TrA in Bracing in maneuver but the difference between positions was not significant in case of measuring TrA activation through AR during bracing. A possible explanation for these results might be that PAR measures TrA activity isolated from other abdominal wall muscles but AR is a measure of activation for TrA alone.
AD targets TrA and therefore spinal stability. However, there is some evidence suggesting that bracing exercises can improve both TrA activity and spinal stability to a better degree (Grenier and McGill, 2007; Hirayama et al., 2017; Vera-Garcia et al., 2007). Comparing the effect of these two maneuvers it was shown that AB can produce better motion control and spinal stability against sudden trunk perturbations (Vera-Garcia et al., 2007). In another study by Grenier and McGill both simulation and in vivo findings show that bracing is superior to AD producing stability (Grenier and McGill, 2007). These findings are also supported by biomechanical studies on the quantification of spinal stability (Grenier and McGill, 2007; Kavcic et al., 2004; McGill et al., 2003). Based on these studies, all trunk muscles must work together to reach spinal stability and stabilization exercises, like AB, should focus on the global coactivation of abdominal muscles to reach this goal. Our study and studies showing the superiority of AB in reaching spinal stability do not diminish the significance of AD maneuver. Rather our findings suggest that the bracing exercises can result in greater TrA activation than AD. The role of AD could be important in late-stage rehabilitation or maintaining spinal stability in higher demand tasks such as sports training (Monfort-Pañego et al., 2009). Previous studies have also shown that TrA might have delayed activity in patients suffering from low back pain which can be treated by drawing-in maneuver (Heidari et al., 2015; Hodges and Richardson, 1998). This might suggest that AB could be more stabilizing in healthy subjects whereas AD is more useful in patients with spinal instability or altered muscle functions.
Our study has several limitations. In this study, we did not calculate the reliability of US but it has been extensively tested and shown to be a reliable tool in measuring TrA thickness (Heidari et al., 2015). The PAR formula that we used in this study may increase the sources of error by taking lateral abdominal wall muscles into account. The error might be more significant particularly in more challenging positions. So, the PAR should be interpreted alongside the more reliable AR formula. In our study most of the subjects were female. It has been previously shown that men tend to have greater TrA thickness than women (Rho et al., 2013; Springer et al., 2006). Women might also have greater thickness percent change of TrA while performing AD (Rho et al., 2013).
There are many proposed core stability exercises in a variety of positions; however, it is not clear that in which position, activation of transverse abdominis muscle is utmost. We compared the effectiveness of drawing-in and bracing maneuvers in different core stability exercise positions (supine, hook lying, supine with 90° flexed knee and hip, supine with stretched knees and 90° flexed hips, bridge, bridge with one stretched knee, and Bird dog) through US imaging. We used transverse abdominis AR as a measure of activation and PAR as a measure of the subject’s ability to isolate the muscle. Our study showed significantly higher activation of transverse abdominis in bridge position and during AB.
REFERENCESDjordjevic O, Djordjevic A, Konstantinovic L. Interrater and intrarater reliability of transverse abdominal and lumbar multifidus muscle thickness in subjects with and without low back pain. J Orthop Sports Phys Ther. 2014;44:979–988.
Ehsani F, Arab AM, Jaberzadeh S, Salavati M. Ultrasound measurement of deep and superficial abdominal muscles thickness during standing postural tasks in participants with and without chronic low back pain. Man Ther. 2016;23:98–105.
Ekstrom RA, Donatelli RA, Carp KC. Electromyographic analysis of core trunk, hip, and thigh muscles during 9 rehabilitation exercises. J Orthop Sports Phys Ther. 2007;37:754–762.
Ferreira PH, Ferreira ML, Hodges PW. Changes in recruitment of the abdominal muscles in people with low back pain: ultrasound measurement of muscle activity. Spine (Phila Pa 1976). 2004;29:2560–2566.
Grenier SG, McGill SM. Quantification of lumbar stability by using 2 different abdominal activation strategies. Arch Phys Med Rehabil. 2007;88:54–62.
Heidari P, Farahbakhsh F, Rostami M, Noormohammadpour P, Kordi R. The role of ultrasound in diagnosis of the causes of low back pain: a review of the literature. Asian J Sports Med. 2015;6:e23803
Hirayama K, Akagi R, Moniwa Y, Okada J, Takahashi H. Transversus abdominis elasticity during various exercises: a shear wave ultrasound elastography study. Int J Sports Phys Ther. 2017;12:601–606.
Hodges PW. Is there a role for transversus abdominis in lumbo-pelvic stability? Man Ther. 1999;4:74–86.
Hodges PW, Moseley GL. Pain and motor control of the lumbopelvic region: effect and possible mechanisms. J Electromyogr Kinesiol. 2003;13:361–370.
Hodges PW, Richardson CA. Delayed postural contraction of transversus abdominis in low back pain associated with movement of the lower limb. J Spinal Disord. 1998;11:46–56.
Hwangbo G, Lee CW, Kim SG, Kim HS. The effects of trunk stability exercise and a combined exercise program on pain, flexibility, and static balance in chronic low back pain patients. J Phys Ther Sci. 2015;27:1153–1155.
Kavcic N, Grenier S, McGill SM. Determining the stabilizing role of individual torso muscles during rehabilitation exercises. Spine (Phila Pa 1976). 2004;29:1254–1265.
Kim BJ, Lee SK. Effects of three spinal stabilization techniques on activation and thickness of abdominal muscle. J Exerc Rehabil. 2017;13:206–209.
Kim M, Kim Y, Oh S, Suh D, Eun SD, Yoon B. Abdominal hollowing and bracing strategies increase joint stability in the trunk region during sudden support surface translation but not in the lower extremities. J Back Musculoskelet Rehabil. 2016;29:317–325.
Koh HW, Cho SH, Kim CY. Comparison of the effects of hollowing and bracing exercises on cross-sectional areas of abdominal muscles in middle-aged women. J Phys Ther Sci. 2014;26:295–299.
Kordi R, Rostami M, Noormohammadpour P, Mansournia MA. The effect of food consumption on the thickness of abdominal muscles, employing ultrasound measurements. Eur Spine J. 2011;20:1312–1317.
Maeo S, Takahashi T, Takai Y, Kanehisa H. Trunk muscle activities during abdominal bracing: comparison among muscles and exercises. J Sports Sci Med. 2013;12:467–474.
Mangum LC, Sutherlin MA, Saliba SA, Hart JM. Reliability of ultrasound imaging measures of transverse abdominis and lumbar multifidus in various positions. PM R. 2016;8:340–347.
Mannion AF, Pulkovski N, Gubler D, Gorelick M, O’Riordan D, Loupas T, Schenk P, Gerber H, Sprott H. Muscle thickness changes during abdominal hollowing: an assessment of between-day measurement error in controls and patients with chronic low back pain. Eur Spine J. 2008;17:494–501.
McGill SM, Grenier S, Kavcic N, Cholewicki J. Coordination of muscle activity to assure stability of the lumbar spine. J Electromyogr Kinesiol. 2003;13:353–359.
McMeeken JM, Beith ID, Newham DJ, Milligan P, Critchley DJ. The relationship between EMG and change in thickness of transversus abdominis. Clin Biomech (Bristol, Avon). 2004;19:337–342.
McPherson SL, Watson T. Reproducibility of ultrasound measurement of transversus abdominis during loaded, functional tasks in asymptomatic young adults. PM R. 2012;4:402–412.
Mishra P, Pandey CM, Singh U, Gupta A, Sahu C, Keshri A. Descriptive statistics and normality tests for statistical data. Ann Card Anaesth. 2019;22:67–72.
Monfort-Pañego M, Vera-García FJ, Sánchez-Zuriaga D, Sarti-Martínez MA. Electromyographic studies in abdominal exercises: a literature synthesis. J Manipulative Physiol Ther. 2009;32:232–244.
Noormohammadpour P, Ansari M, Mansournia MA, Rostami M, Nourian R, Kordi R. Reversal time of postprandial changes of the thickness of abdominal muscles employing ultrasound measurements. Man Ther. 2015;20:194–199.
Noormohammadpour P, Kordi R, Dehghani S, Rostami M. The effect of abdominal resistance training and energy restricted diet on lateral abdominal muscles thickness of overweight and obese women. J Bodyw Mov Ther. 2012;16:344–350.
Noormohammadpour P, Kordi M, Mansournia MA, Akbari-Fakhrabadi M, Kordi R. The role of a multi-step core stability exercise program in the treatment of nurses with chronic low back pain: a single-blinded randomized controlled trial. Asian Spine J. 2018;12:490–502.
Panjabi MM. The stabilizing system of the spine. Part I. Function, dysfunction, adaptation, and enhancement. J Spinal Disord. 1992;5:383–389.
Rho M, Spitznagle T, Van Dillen L, Maheswari V, Oza S, Prather H. Gender differences on ultrasound imaging of lateral abdominal muscle thickness in asymptomatic adults: a pilot study. PM R. 2013;5:374–380.
Rostami M, Ansari M, Noormohammadpour P, Mansournia MA, Kordi R. Ultrasound assessment of trunk muscles and back flexibility, strength and endurance in off-road cyclists with and without low back pain. J Back Musculoskelet Rehabil. 2015;28:635–644.
Selkow NM, Eck MR, Rivas S. Transversus abdominis activation and timing improves following core stability training: a randomized trial. Int J Sports Phys Ther. 2017;12:1048–1056.
Springer BA, Mielcarek BJ, Nesfield TK, Teyhen DS. Relationships among lateral abdominal muscles, gender, body mass index, and hand dominance. J Orthop Sports Phys Ther. 2006;36:289–297.
Teyhen DS, Miltenberger CE, Deiters HM, Del Toro YM, Pulliam JN, Childs JD, Boyles RE, Flynn TW. The use of ultrasound imaging of the abdominal drawing-in maneuver in subjects with low back pain. J Orthop Sports Phys Ther. 2005;35:346–355.
Vera-Garcia FJ, Elvira JL, Brown SH, McGill SM. Effects of abdominal stabilization maneuvers on the control of spine motion and stability against sudden trunk perturbations. J Electromyogr Kinesiol. 2007;17:556–567.
Fig. 1Training position: (A) supine, (B) Hook lying, (C) 90° flexed knee and hips, (D) stretched knees and 90° flexed hips, (E) bridge, (F) bridge with one stretched knee, and (G) bird dog. These figures are presented with the consent of the subject. 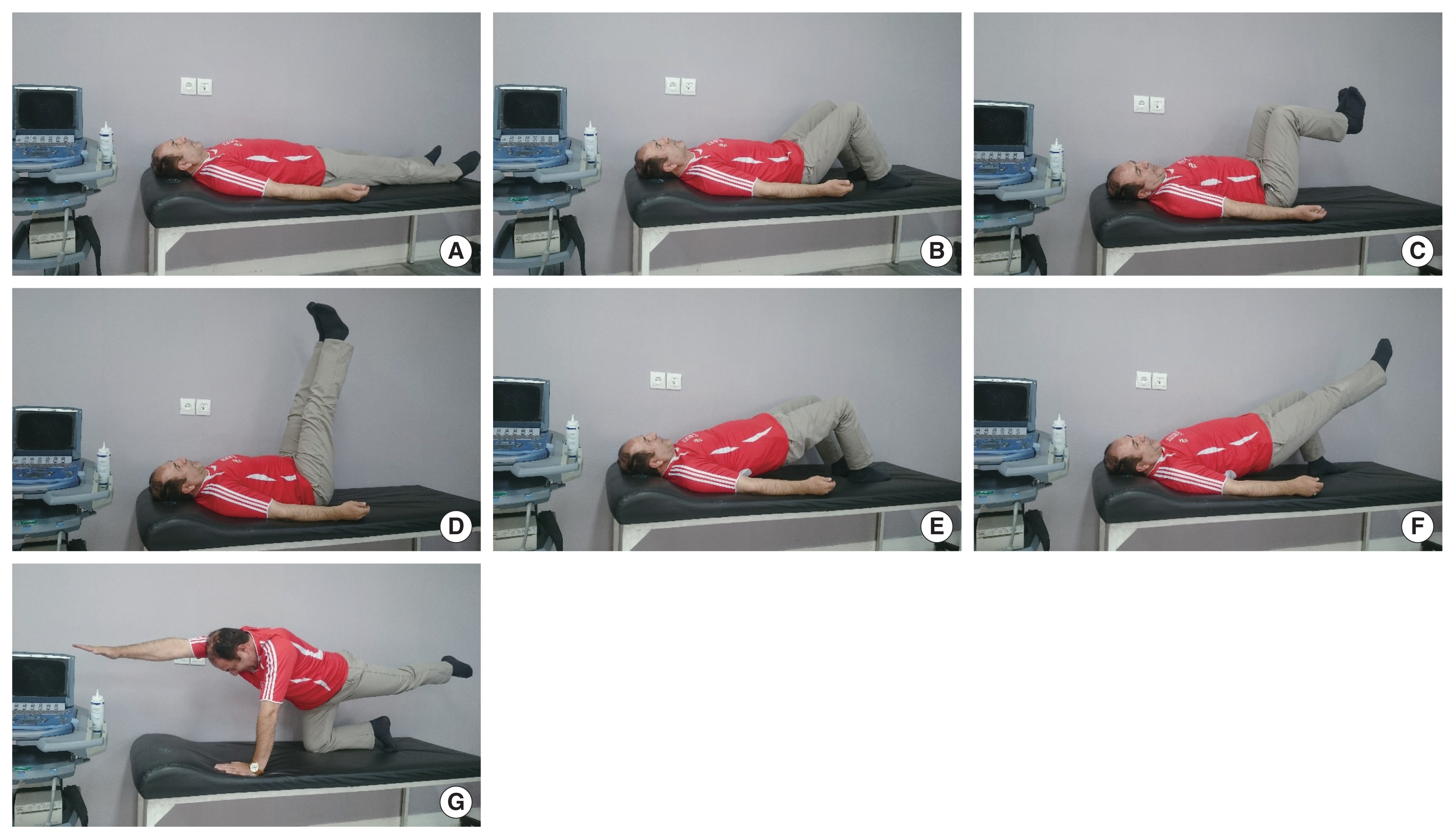
Fig. 2Recruitment of transverse abdominis in each training position. (A) Activation ratio, (B) preferential activation ratio. 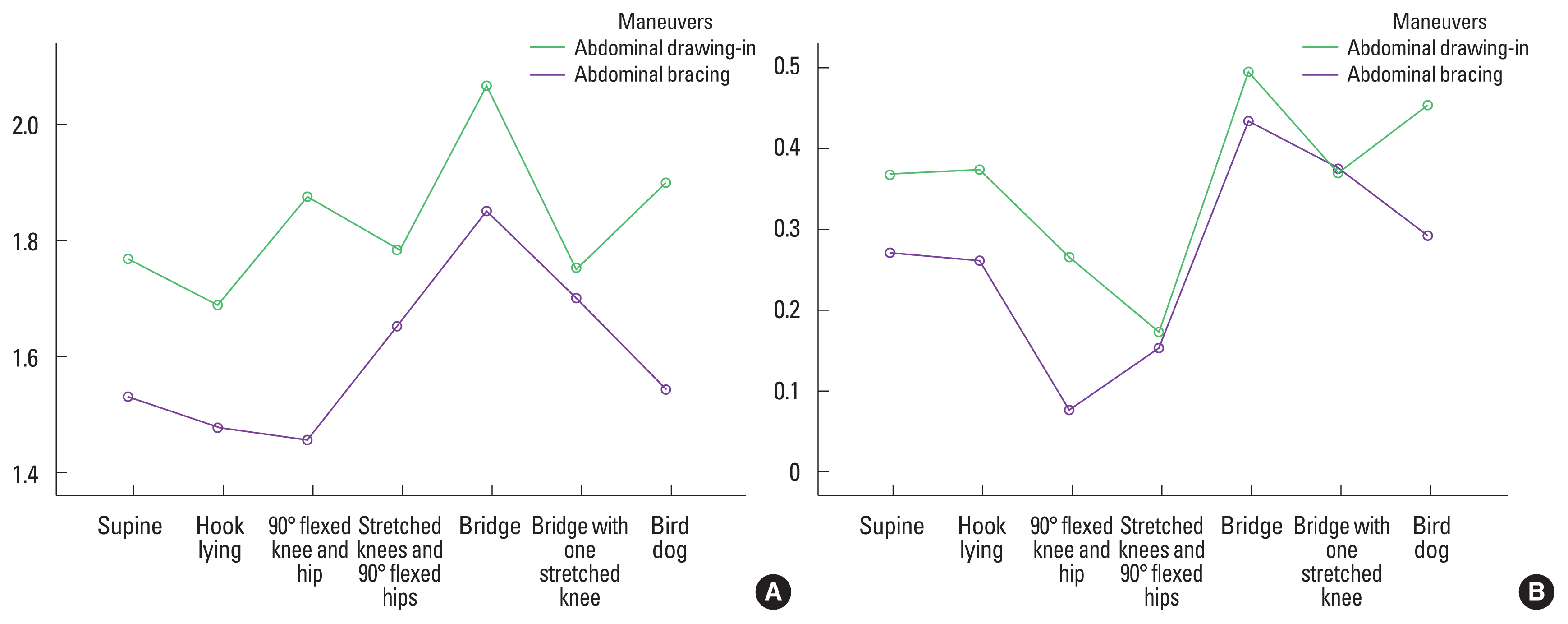
Table 1Descriptive characteristics of study subjects
Table 2The thickness of TrA during rest, abdominal drawing-in, and abdominal bracing in different training positions
Table 3Activation measures of TrA in different core training positions
|
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||