INTRODUCTION
According to the 2013 mortality rate data, more than 2,200 Americans die every day due to cardiovascular disease (Mozaffarian et al., 2016). This disease disrupts the vascular system as well as having the potential to damage the body’s vital organs including the heart and brain (Basson, 2008). It has been reported that performing moderate-intensity exercise 2 days a week for 30 min may reduce the mortality risks from cardiovascular disease in sedentary obese adults (Apekey et al., 2012). Those who do not participate in any form of exercise may start with a simple and safer activity such as walking to increase their fitness level (Wen et al., 2014). Accordingly, walking durations of 30 min are considered an aerobic or cardiorespiratory form of exercise and could be modified to an activity with higher intensity (Graves et al., 1987).
In previous studies, intensity was shown to be a key component in how energy levels are affected during the exercise one participates in, especially while walking with hand-held weights (HHW) (Evans et al., 1994; Morrow et al., 1992; Owens et al., 1989). Key factors contributing to the caloric expenditure and exercise intensity from walking while moving HHW were arm range of motion and walking speed (Morrow et al., 1992). However, another investigation reported intensity is enhanced through both carrying HHW and greater arm range of motion (Makalous et al., 1988). Other studies also reported arm motion is crucial for increasing energy cost (Auble et al., 1987; Maud et al., 1990). Two studies had arms begin at the sides and moving hands up to waist level 90° (Makalous et al., 1988; Zarandona et al., 1986). One used a normal arm range of motion (Owens et al., 1989) while another used normal arm swings while hands passed the shoulder and behind the gluteus maximus for vigorous arm swings (Maud et al., 1990). Others lifted to shoulder height while the opposite elbow flexed at 90° (Graves et al., 1987) or lifted 30.48 cm forward and upward exceeding 90° elbow flexion (Knowlton et al., 1992) Additionally, carrying 1.36 kg HHW was needed to significantly increase metabolic costs during the exercise (Knowlton et al., 1992; Zarandona et al., 1986).
Excess post-exercise oxygen consumption (EPOC) is the elevated postexercise metabolism which adds to the energy expenditure (EE) of the exercise and as a component of the thermic effect of the activity (Laforgia et al., 2006). Two energy systems, phosphocreatine and anaerobic glycolytic systems, provide sources of energy to the body while exercising (Chandler and Brown, 2012). When these energy supplies deplete during exercise, the oxidative system mainly supplies energy for the body, whereas EPOC replenishes the anaerobic system postexercise (Chandler and Brown, 2012). To our knowledge, no study has investigated the effects of treadmill walking with HHW that specifically based the intensity at a moderate level of 40%–59% using the Karvonen heart rate (HR) reserve method, nor examined its effects on EPOC. Therefore, the purpose of this study was to compare the physiological responses in sedentary women between treadmill walking with versus without 1.36 kg HHW at a moderate level of intensity on EE, oxygen uptake (VO2), HR, amount of fat and carbohydrates (CHO) expended, respiratory exchange ratio (RER), rating of perceived exertion (RPE), and EPOC.
MATERIALS AND METHODS
Participants
Nineteen college-age women, mean±standard deviation, 21±2.7 years old, 66.61±15.11 kg, and 163.1±6.3 cm tall, volunteered and completed the research study. The study focused on women because this population seemed to engage more often in walking with HHW compared to men. In addition, male participants were more prevalent participants in previous studies compared to females. Physical characteristics of the participants are summarized in Table 1.
The participants were either sedentary or had not taken part in any exercise within the previous six months prior to participation. Exclusion criteria included having hypertension or other cardiovascular medical conditions that would prevent them from being capable to participate in the study. No medication was used by the participants that affected their HR or blood pressure. Participants were also not allowed to consume caffeine or alcohol 24 hr before the testing sessions and fasted for at least one hour with the exception of water before the testing began. The attire worn during the study was comfortable exercise clothing and tennis shoes. This study was approved by the Institutional Review Board of California State University, Fullerton (approval number: HSR-15-0275). An informed consent document was given to each participant who signed prior to participating in the study.
Research design
Sedentary or untrained women volunteered for the study and visited the laboratory on two randomly-ordered sessions. Both sessions consisted of one exercise protocol and an EPOC period that lasted for approximately 1 hr combined. The two sessions were completed at least one day apart and were randomly ordered to have the participant move their arms either with 1.36 kg HHW or without HHW during treadmill walking.
During the first visit, the participant was seated and given an informed consent to read the procedures and sign to agree to the conditions of the study. A Pre-Exercise Testing Health & Exercise Questionnaire was also given for the participant to complete to make certain her health status was suitable for the study. If acceptable, the next appointment was scheduled. Then, the participant’s resting HR was taken after at least 10 min of seated rest by relaxing her arm in a supine position and using the tips of four fingers, excluding the thumb to press onto the radial artery of the thumb side of her wrist (Yim and Park, 2014). When the pulse was felt, HR was assessed for 1 min and then recorded (Yim and Park, 2014). The maximum HR prediction was calculated using the formula: HRmax=192−(0.007×age2) (American College of Sports Medicine [ACSM], 2014). To calculate maximum HR reserve the following formula was used: HRreserve=HRmax−HRrest (Graves et al., 1987). Moderate intensity was set between 40%–59% (ACSM, 2014). The target HR (THR) was calculated using: THR40%=HRrest+ 0.40 (HRmax−HRrest) and THR59%=HRrest+0.59 (HRmax−HRrest) (Kenney et al., 2012).
Next, the anthropometrics of each participant were measured, which consisted of their body mass, height, and body composition. First, the participant removed her shoes before stepping onto the digital scale (Ohaus ES Series scale, Parsippany, NJ, USA) where her body mass was measured and recorded in kg. Then, with her shoes removed, she stood tall against the stadiometer (Seca stadiometer, Chino, CA, USA) and after the participant took one deep breath, her height was measured in cm. To obtain the circumferences of the hip and waist, a spring-loaded tape measurer (Gulick-Baseline Evaluation Instruments tape measurer, Knoxville, TN, USA) was used to measure the areas in centimeters. The waist was measured around the narrowest portion between the ribs and the hip bone (ACSM, 2014). The hip was measured on the widest portion around the hips and the gluteus maximus (ACSM, 2014). The waist-to-hip ratio was calculated by dividing the hip by the waist in cm (ACSM, 2014).
In addition to the waist-to-hip ratio, the participant’s body fat (BF%) was measured with a skinfold caliper (Harpenden Skinfold Caliper, Sussex, England) using the Jackson and Pollock 7-site method (ACSM, 2014). The seven sites included the chest, subscapular, midaxillary, triceps, abdominal, suprailiac, and thigh folds (ACSM, 2014). Body density (DB) was calculated using: DB =1.097−(0.00046971×sum of seven skinfolds)+[0.00000056× (sum of seven skinfolds2)−(0.00012828×age)] (ACSM, 2014). Then, the BF% was calculated using the Siri equation: BF%= (495÷DB)−450 (ACSM, 2014). Fat body mass which is the mass of the BF% was calculated as: fat body mass=(BF%×body mass) ÷100 (Siri, 1993). The lean body mass was calculated by taking the difference between the body mass and the fat body mass (Siri, 1993).
After all skinfolds were taken, the participant was instructed on proper arm and leg motion. The correct arm motion for the current study was to flex 90° at the elbow (about waist level), while alternating each arm forward and backward (Evans et al., 1994). Both elbows were constantly flexed throughout the entire exercise trial and alternated approximately 30.48 cm forward and 30.48 cm backward from the waist (Evans et al., 1994). As the arm motion was performed, the opposite leg was to be in front with the opposite arm (elbow flexing at 90°) in front (Auble et al., 1987; Evans et al., 1994).
During extensive piloting, moving 2.27 kg HHW was too challenging for the moderately active to very active participants as they were unable to complete the entire 30 min of physical activity at the prescribed motion. To avoid increasing the risk of pain and injury of the participants, less heavy weights were used for the women who do not exercise. Thus, the sedentary women used 1.36 kg HHW during the current investigation. The participants’ arm range of motion was measured through close observations by the investigator. If failing to meet the prescribed motion, verbal communication was given to assist participants in correcting their arm range of motion.
The Borg RPE scale was explained to the participant such that she could point to a number on the scale during the exercise test (ACSM, 2014). The participant was equipped with a HR monitor and a mouthpiece, which held in place a two-way rebreathing valve (Hans-Rudolph Inc., Shawnee, KS, USA). The rebreathing valve, where respiratory gases were collected, and mouthpiece were also attached to a headgear. Participants wore a nose clip to ensure that breathing occurred entirely through the mouth.
Then the participant sat for 5 min with the equipment remaining attached for the baseline period. After 5 min of quiet sitting, the participant transferred to the treadmill where she performed a 5-min warm-up with the arm and leg motion described previously, as the treadmill intensity was gradually increased. Based on the American College of Sports Medicine, the intensity recommendation was to be constant (ACSM, 2014). The speed of the treadmill was adjusted to match a moderate level of the THR of the participant and treadmill grade was raised to 1% to mimic outdoor walking. The exercise was performed after the warm-up, which was when the participant walked with the specified motion for 30 min. This was the control exercise trial without HHW. When the participant completed the exercise test, she sat on a chair for 30 min to have these same measurements assessed during the EPOC period.
Treadmill speed and RPE based on the Borg scale was obtained every 5 min during the exercise test. EE, fat expenditure, CHO expenditure, VO2, RER, and HR were collected every min throughout the entire exercise test and EPOC period using a calibrated metabolic cart (Parvo Medics TrueOne 2400 Metabolic Measurement System, Sandy, UT, USA). The metabolic cart was calibrated prior to each test with room air and standard gases of known volume and concentration for the oxygen (O2) and carbon dioxide (CO2) analyzers. O2 and CO2 were analyzed through a sampling line after the gasses passed through a heated pneumotach and mixing chamber.
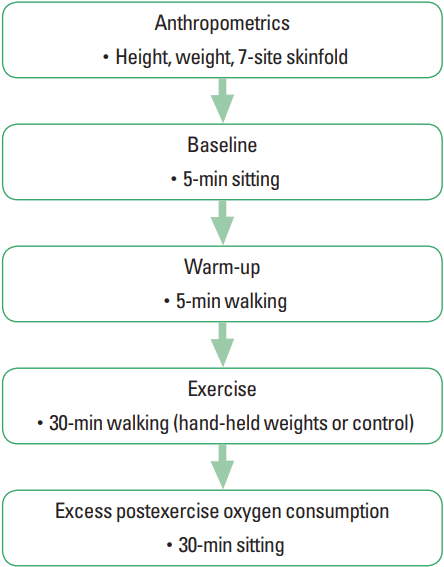
For the second visit, the participant’s resting HR was recorded in the same manner as the first visit. The participant practiced the specified arm and leg motion used in the first visit while lightly grasping and moving the 1.36 kg HHW. The 1.36 kg HHW (Tone Fitness, Houston, TX, USA) were secured with velcro straps to the participant’s hands to help hold the HHW in place such that the participants would not have to be concerned with the HHW sliding or falling. Once comfortable with the motion, the participant sat for 5 min with the HR monitor, nose, head, and mouth equipment pieces attached. Following the 5-min baseline period, the participant performed a 5-min warm-up on the treadmill with the specified motion learned and the intensity was gradually increased. Next, the exercise test began for 30 min with the arm and leg motion and with 1.36 kg HHW. In both visits, instruction was given to remind the participant of the proper arm and leg motion, if needed. EE, fat expenditure, CHO expenditure, VO2, RER, treadmill speed, RPE, and HR were collected in the same manner as the first visit. When the exercise test was completed, the participant sat on a chair for 30 min for EPOC to be measured. Fig. 1 summarizes the overall research design of the study.
Statistical analysis
EE, fat expenditure, CHO expenditure, HR, VO2, RER, treadmill speed, and RPE responses were evaluated using multiple two-way analysis of variance (ANOVAs) (time×condition) to compare the two different conditions of HHW and control. In the two-way ANOVA, if an F was significant, one-way ANOVAs and post hoc Tukey tests were used when appropriate to determine which mean differences were significant. An alpha level of P≤0.05 was considered to be statistically significant. All statistical analyses were conducted using IBM SPSS Statistics ver. 23.0 (IBM Co., Armonk, NY, USA).
RESULTS
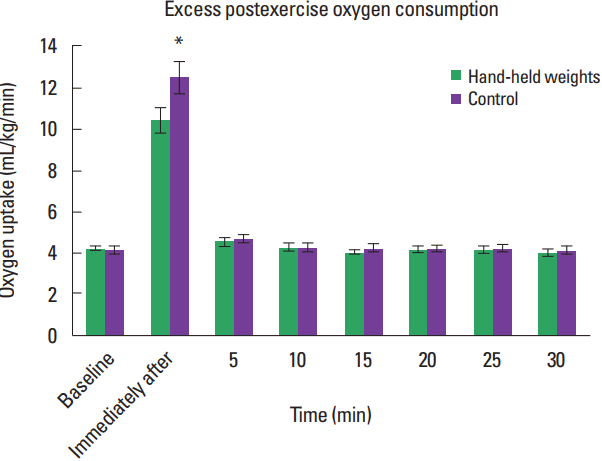
There was a main effect for time for EPOC (F=165.253, P≤ 0.001). Pairwise comparisons collapsed across conditions indicated relative VO2 (mL/kg/min) was 176.8% higher immediately after exercise compared with baseline (P≤0.001) as shown in Fig. 2. No other significant differences were found among other time points during EPOC (P>0.05).
Overall, there were no significant differences for EE (F=2.946, P=0.103), fat expenditure (F=0.01, P=0.92), CHO expenditure (F=0.319, P=0.579), VO2 (F=0.319, P=0.579), RER (F=0.034, P=0.855), or HR (F=3.395, P=0.082) between conditions during the exercise (P>0.05). There was a main effect for condition for treadmill speed (F=23.711, P≤0.001). Speed was 11.5% higher for the control compared to the HHW condition. In addition, there was a main effect for condition for RPE (F=28.551, P≤0.001). RPE was 9.91% higher for the HHW compared to the control condition. Fig. 3 displays VO2 during the exercise. The mean and standard error for each variable collected during the study are displayed on Table 2.
DISCUSSION
The main result of this study was a significant difference during EPOC for EE, which lasted no longer than 5 min after the end of the exercise. Although the EE was significant immediately after 5 min of exercise, EPOC did not remain elevated for a longer period. An explanation for this may be due to the controlled moderate-intensity of the treadmill walking exercise. Climactic increases in VO2 occurred with increasing walking speed rather than adding HHW at a fixed speed (Owens et al., 1989). In general, walking with HHW decreased the intensity of normal walking while the participant was walking on the treadmill (Morrow et al., 1992). It appears that a sufficient arm motion with a greater HHW load will increase the EE; however, this was influenced with a slower pace of walking, thus decreasing the walking speed (Morrow et al., 1992).
Since the treadmill speed was adjusted to match HR with a moderate intensity between 40%–59%, there may not have been any additional EE benefits because HR, VO2, and REE are linearly related to the workload (Zarandona et al., 1986). Instead, the current investigation supported the findings from another study that reported no additional benefits were obtained from carrying HHW with a constant THR intensity (Evans et al., 1994). The study compared a self-chosen pace and altered HR intensity at 70% HRreserve across conditions with 0, 0.45, 1.36, and 2.27 kg in older adults (Evans et al., 1994). The arm range of motion was nearly identical with 90° elbow flexion; however, the current study specified arms to move 30.48 cm forward and backward whereas the previous study used normal arm movements (Evans et al., 1994). Maintaining a constant THR resulted in similar EE (no differences in VO2, VE, RER, and RPE) with different HHW volumes or weight levels (Evans et al., 1994).
On the contrary, an advantage of using THR is that the metabolic demand remains the same despite decreasing speed and increasing volume of weight carried (Evans et al., 1994). The current investigation for the HHW condition resulted in a 12.9% lower treadmill speed and a higher RPE by 9.9% compared to the control condition. This particularly helps older adults or those who are working to achieve a training level to meet their THR without having to walk faster (Evans et al., 1994; Graves et al., 1987; Zarandona et al., 1986). More HHW volume contributes to stressing the body which may help adults to eventually increase their walking speed through training and after the removal of HHW.
While there were no additional EE benefits observed in this study during the exercise, another investigation reported benefits from walking with HHW (Evans et al., 1994). For instance, patients with myocardial infarction had improved ischemic thresholds when walking with HHW (Evans et al., 1994). It was suggested by the researchers that patients with myocardial infarction who walk while moving HHW had small increases in diastolic blood pressure which caused effusion of the blood flow and consequently increased the myocardial oxygen supply (Evans et al., 1994).
To our knowledge, no study has examined sedentary or untrained women, and included 5 min of sitting, a warm-up, and 30 min of exercise followed by subsequent quiet sitting for 30 min. In addition, participants’ arm range of motion, alternating 30.48 cm forward and backward while maintaining elbow flexion (bent) at 90° for both sessions during the warm-up and exercise, was not examined in other studies.
Individuals casually walk with weights as part of their physical activity to increase the amount of calories expended. However, walking with 1.36 kg HHW for 30 min between 40%–59% of their THR was not enough to achieve greater EE during the exercise. Since EE was not significantly different, individuals may want to consider walking at more vigorous intensities or varying their HR training zones.