INTRODUCTION
The shoulder is the most frequently dislocated joint in the human body, anterior dislocation is the most common injury in our daily life, especially for young people (Liu et al., 2014; Rumian et al., 2011). It was estimated that the incidence rate of shoulder dislocation is 23.9 per 100,000 persons a year (Owens et al., 2009). Anterior shoulder dislocations and subluxations are common injuries in young athletes (Kaplan et al., 2005; Malhotra et al., 2012). The disparity between the large humeral head and the small glenoid cavity increasing the joint ability to be injured (Brandt et al., 2013; Brukner and Kham, 2012). Moreover, the anteriorly dislocated humeral head causes a labrum tear of the anterior and inferior labrum, a Bankart injury (Longo et al., 2014; Porcellini et al., 2009), and a typical impression fracture (Hovelius et al., 2008; Kim et al., 2003).
The mechanism of the first dislocations occurs after a forceful direct trauma or a fall typically with the arm in an abducted and externally rotated or outstretched arm (Owens et al., 2010). Thus, in the majority of cases, the arm is abducted and the shoulder is externally rotated (Hardy et al., 2010). This is common in rugby, hockey, Handball, Football, riding, and cycling. In patients with lax shoulders or previous dislocations, dislocation can occur after much less trauma (Badr and Gaballah, 2015; Brooks et al., 2005; Kelly and Terry, 2001). Recently, the most common management of treatment for primary anterior glenohumeral instability is non-operative management (Gibson et al., 2004; Zacchilli and Owens, 2010). Rehabilitation and prevention of this injury are worthwhile of research because the negligence of rehabilitation for the first-time dislocation shoulder may lead to recurrent instability of the glenohumeral joint (Provencher et al., 2010; Rumian et al., 2011). Furthermore, there is a body of reports suggesting that younger athletes generally and contact sports particularly are most affected with an instability risk after a primary anterior shoulder dislocation (Handoll et al., 2006; Zacchilli and Owens, 2010). This risk of the recurrence dislocation reported in young athletes with first-time anterior dislocation is high as 90%–95% (Gibson et al., 2016). However, the athletes with anterior shoulder dislocation who returned to activities within the season after lack rehabilitation have demonstrated high rates of recurrent dislocation from 37% to 90% (Castagna et al., 2007; Watson et al., 2016). The goal of the primary rehabilitation for the acute anterior shoulder is to prevent long-term instability for the shoulder joint (Leroux et al., 2014). However, patients with recurrent shoulder instability often need a surgical intervention or arthroscopic treatment (Malhotra et al., 2012; Porcellini et al., 2009; Provencher et al., 2010). Indeed, several modalities used conservative treatment for the acute dislocation shoulder (Liavaag et al., 2011; Liu et al., 2014; Yamamoto et al., 2010) and injections (Nagata et al., 2015). Some approaches have conducted physical rehabilitation programs for a first-time shoulder dislocation (Gibson et al., 2004; Karatsolis and Athanasopoulos, 2006; Salamh and Speer, 2013). Other used the elastic resistance exercise which has become one of the popular tools in physical rehabilitation (Andersen et al., 2010; Brandt et al., 2013; Camci et al., 2013). The major reason to use the elastic band is that they have demonstrated excellent validity and reliability with shoulder muscle testing (Andersen et al., 2016). Ultimately, the aim of this study is to design a physical rehabilitation program using an elastic band and resistive exercise to improve joint strength in individuals diagnosed with a first-time shoulder dislocation.
MATERIALS AND METHODS
Subjects
Physically active males who came to Mansoura University Hospitals and the teaching hospital in Damietta, Egypt with acute anterior dislocation shoulder injury between September 2013 and February 2016 were randomly recruited as research participants. Magnetic resonance imaging was conducted to determine the injury grade for 17 athletes. Furthermore, excluded the patients with recurrent dislocation shoulder or with a history of injury in the same joint. Twelve physically active males (age, 18.6±1.32 years; mass, 74.48±3.22 kg; height, 178.4±3.21 cm with competitive experience 9.6±2.67 years) and first-time acute shoulder dislocation were considered as research participants. The participants began a physical rehabilitation program 2 weeks after the shoulder dislocation, which was confirmed by a referring physician.
Rehabilitation program
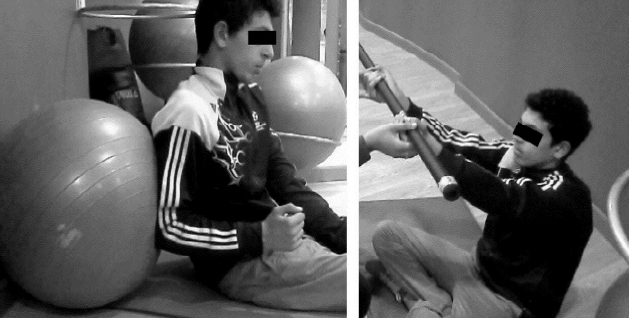
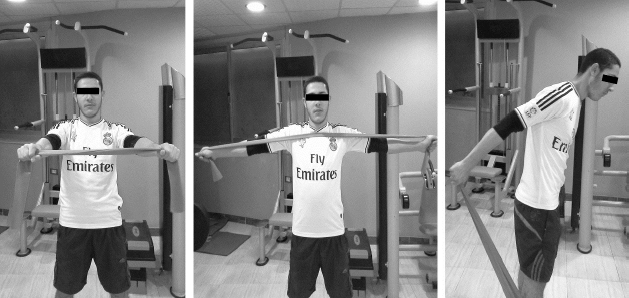
The duration of the rehabilitation protocol was 6 weeks and was divided into three stages. However, the duration of each stage was 2 weeks. Seventeen external and internal rotation exercises were chosen for the first stage which aimed to control the pain and inflammation caused by the dislocation. Also, was included flexibility and isotonic strength exercise with 12–15 reps and 30% intensity of one-repetition maximum (1RM) for the healthy shoulders. Which performed for the scapulothoracic muscles, in particular, the rotator cuff muscles (Fig. 1). The second stage aimed to restore the higher level of muscle strength. The intensity of exercises was five sets with 8–10 reps and 60%–70% of 1RM for the healthy shoulders. Thirty-two exercises were performed in the second stage. In particular, Deltoid M., Trapezius M., and Serratus Anterior M. exercises in this stage were performed widely in the horizontal and diagonal axes. Moreover, the exercises were chosen to enhance the range of motion (ROM) and muscles strength between 90°–150° vertically, horizontally, and diagonally (Fig. 2).
The third stage was designed for the endurance, plyometric, and strength exercises and was consisted of five sets of with 3–6 reps using variable resistance: one at 75% of the 10RM, and two at 95% of the 1RM. Twenty-seven extremity weights rehabilitation exercises were performed to reach 190°–200° ROM and the equally healthy arms strength as well (Fig. 3). The Thera-Band resistance exercises were used during the six weeks especially the four colors (red, blue, black, silver, and gold). The red and blue bands are used in the first stage and the black and silver used in the second stage, In addition, the gold was used in the third stage. Furthermore, all the exercises performed by stretching the band between 75%–100%. knowing that, the weight of stretching the Thera-Band between 75%–100% is (red, 3.3–3.9; blue, 5.9–7.1; black, 8.1–9.7; silver, 11.1–13.2; and gold, 18.1–21.6 kg) (Andersen et al., 2010; Biçer et al., 2015).
Data collection
The rehabilitation program comprised four testing sessions. The pretest section was conductedth after 2 weeks of the injury and before the beginning of the rehabilitation program. After two rehabilitative weeks, the 2nd-week tracking test was realized, while the 4th-week tracking test was realized after the 4th rehabilitative week. Moreover, after a resting of six weeks, posttest was collected. Additionally, all the injured athletes were right handed and in each test, the healthy arms measurements were recorded. Continuously, the test results for the injured arm had been compared with the healthy arm for each person. Before reporting the force measurement, all the participants were informed of the test procedures for both arms. Four basics Isotonic force measurements were reported by an Isometric Dynamometer device (Isokinetic Dynamometer, BiodexMedical Systems, Shirley, NY, USA). These force measurements were conducted for muscles around shoulder girdle in the 90°, vertically and horizontally. The force variables were flexion force (FF), adduction force (ADF), abduction force (ABF), and hyperextension force (HBF). The participants were asked to perform the maximum flexibility for the shoulder joint without feeling pain. In addition, the ROM variables were obtained by goniometer for flexion ROM (F.ROM), abduction ROM (AB.ROM), and hyper extension ROM.
Data analyze
The paired t-test was used to compare the collected data before performing the exercise protocol (pretest) and those which were obtained after 6-week physical rehabilitation period (posttest). All the analyses were performed by using IBM SPSS Statistics ver. 19.0 (IBM Co., Armonk, NY, USA). Additionally, all values within the text and table are observed as standard deviation and mean.
RESULTS
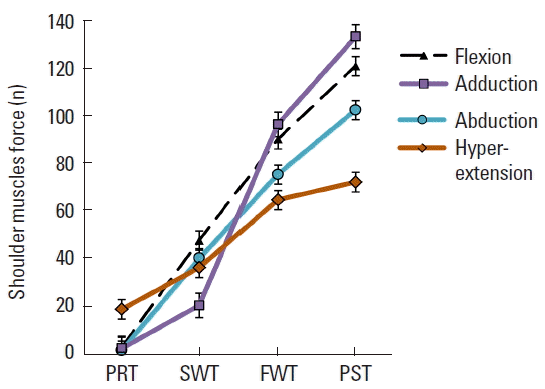
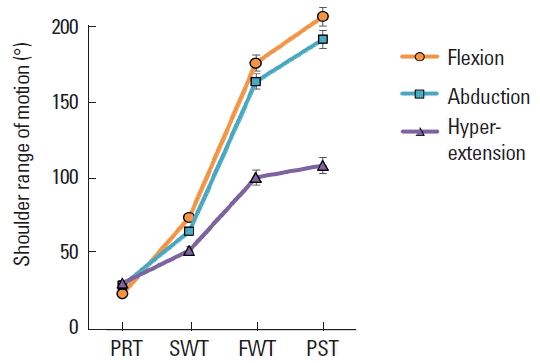
The test results (i.e., strength and ROM) show that there were no statistically significant differences between the injured and uninjured shoulder (P>0.01) prior to the rehabilitation procedure. After 6-week physical rehabilitation, the test results showed considerable improvement of more than 90%. The difference between the pretestes and posttests of force were, FF 4.41±4.01 vs. 121.5±12.4, ABF 2.94±2.74 vs. 103.1±9.8, ADF 3.84±0.34 vs. 133.7±9.26, HBF 20.01±7.64 vs. 69.1±8.92 (Fig. 4). On the other hand, the ROM of pretestes and posttest were, FF 23.8°±4.02° vs. 199.5°±0.24°, ABF was 29.3°±3.62° vs. 195.5°±2.13°, HBF 30.8°±5.81° vs. 108.5°±5.72°. Furthermore, the conducted post tests have shown that there were no significant differences (P<0.53) between the shoulder muscle force for the injured and uninjured shoulders. However, the participants’ injured shoulder showed great improvement after the rehabilitation (Fig. 5).
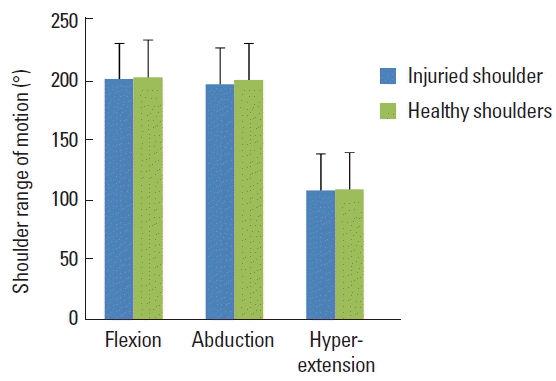
In addition to the posttests of the injured compared with the uninjured shoulders were, FF 121.5±12.44 vs. 128.2±10.4 with 94% enhancement, ABF 103.1±9.81 vs. 110.9±8.32 was 93% enhancement, ADF 133.7±9.26 vs. 135.2±5.33 with enhancement 99%, HBF 69.1±8.92 vs. 72.71±5.42 with 95% enhancement (Fig. 6). In contrast, F.ROM 199.5°±0.24° vs. 201.3°±1.25° was 99% enhancement, AB.ROM 195.5°±2.13° vs. 198.9°± 1.06° had 98.3% enhancement, and HE.ROM 107.8°±6.12° vs. 108.5°±5.72° was 99.4% enhancement (Fig. 7). Finally, the rehabilitation did not induce any side effects: muscle atrophy changes and swells were not detected.
DISCUSSION
The current study aimed to design a rehabilitation program used the elastic and weights exercises. Over the past decades, we have seen a huge boost in the rehabilitation of shoulder dislocation injuries. These injuries occurred because of the anatomical structure of the glenohumeral joint. Therefore, derives its extensive movement at the expense of its consistency and coherence. More than 50% of acute anterior dislocations can reoccur, especially in young athletes. The aim of the physical rehabilitation is avoiding the recurrent dislocation and using an elastic band and resistive exercise to improve joint strength in individuals diagnosed with a first-time shoulder dislocation.
The current study results show that there was weakness of the shoulder muscles in the pretest measurements of FF, ADF, ABF as a result of pain, swelling, and inflammation. Nevertheless, the hyperextension motion measurements were reported better than the other measurement in the pretest. The mechanism of the anterior dislocation occurred forwardly and downward. Out of the ordinary, that affected adversely on the forward movement of the arm (Turkel et al., 1981)
The return to activity after 2–3 weeks is available for athletes with a high risk of recurrence dislocation, which compares to arthroscopic remain and return to activity after a 6-month surgical stabilization (Watson et al., 2016). Many factors have been related to rehabilitating shoulder dislocation. Thus, the current study concluded that six weeks’ elastic resistant with weight exercise had great benefit for the shoulder muscles especially, the Rotator Cuff muscles. Recently, the popularity of elastic bands has increased because of their low prices, flexibility, adaptability, versatility, and simplicity (Andersen et al., 2010; Jakobsen et al., 2013). The incorporation between Nautilus machine and the elastic band’s exercises have been used to promote the joint ROM and muscles strength in training and rehabilitation purposes as well. Thus, the elastic resistant exercise has improved the strength-shorting cycle. In addition, it has been used as a technique to produce the speed eccentric contraction (Stevenson et al., 2010).
It is seen in Figs. 4 and 5. that there is a considerable significant difference between the pretests and the posttests of the injured shoulders. Also, it is seeming to be similar to the healthy shoulder after the six weeks’ physical rehabilitation program (Fig. 6). The same resulted reported in a previous study conducted on young handball players and has improved their muscle power, muscle strength and ball speed (Mascarin et al., 2016). Nevertheless, the elastic resistant and free weight exercise improve the dynamic stabilization and joint stability (Andersen et al., 2010; Camci et al., 2013). Thus, the exercise rehabilitation program for the unstable shoulder must include a joint position sensibility and dynamic stabilization to support the functional stability of the shoulder joint and promoted the co-activation of the force couples about the glenohumeral joint to exceptional position of the hummers head in the center of glenoid (Naughton et al., 2005).
Previous studies have demonstrated same levels of muscle activation using elastic resistance compared with free weights and display similar or even greater levels of muscle activity for some muscles during an exercise (Andersen et al., 2010; Camci et al., 2013). In contrast, used with the free weights (Aboodardaa et al., 2013). Other studies have shown high levels of muscle activation compared with weight machine (Brandt et al., 2013). But all the modalities recommended use of the elastic band with the weights. Moreover, using the elastic band with weights appear to be equally in muscle activity as a traditional use of isoinertial resistance (Jakobsen et al., 2013). Finally, the physical rehabilitation program proposed in this study was effective at improving strength and ROM in the injured shoulder as evidenced by the similarity in posttest values between the injured and uninjured shoulder. These results are encouraging and suggest the physical rehabilitation program proposed in this study may help reduce the need for surgical intervention in healthy young males who experience a primary shoulder dislocation.